The Dynamic
Resilience
System™
A five-stage integrated approach to injury recovery and long-term physical resilience — combining physiotherapy, chiropractic and exercise physiology into one coordinated plan.
Why most recovery
doesn’t stick.
The most common failure in musculoskeletal healthcare is not inadequate treatment — it is incomplete treatment. Most patients receive care that effectively reduces their pain. They feel better. They stop coming. And within weeks or months, the same problem returns.
This happens because pain relief and recovery are not the same thing. When treatment ends at symptom resolution, the underlying deficits — reduced strength, poor load tolerance, altered movement patterns — remain unaddressed. The alarm has been silenced, but the system has not been fixed.
The Dynamic Resilience System™ was developed to break this cycle — by treating recovery as a process, not an event.
Standard Care
- Reactive — treats symptoms as they arise
- Ends at pain relief
- Time-based progression
- Siloed disciplines
- Symptom-focused discharge
Dynamic Resilience System™
- Progressive through defined stages
- Continues to full function & resilience
- Criteria-based progression
- Integrated physio, chiro & EP
- Capacity-based, goal-driven discharge
Five stages.
One coordinated plan.
Each stage builds on the last. Every transition is based on measurable clinical milestones — not time elapsed, and not pain level alone.
The Five Stages
Each stage builds on the last. Every transition is based on measurable clinical milestones — not time elapsed, and not pain level alone. From your first assessment through to long-term resilience, the System is designed to take you further than pain-free.

“A thorough assessment of your injury, movement, history and goals — so treatment is built on understanding, not assumption.”
Before any treatment begins, we need to understand exactly what is happening — and why. The Review stage is a comprehensive clinical assessment covering your pain, movement quality, strength, load tolerance and the factors in your life that may be influencing your recovery.
Goals
- Identify source & contributing factors
- Establish functional baseline
- Screen for red flags
- Understand your goals & demands
- Build a personalised treatment plan
What This Involves
- Full musculoskeletal assessment
- Movement screening & neural testing
- Biopsychosocial screening
- Validated outcome measures
- Goal-setting & planning discussion
Next stage when: The clinical picture is clear and a treatment plan has been established. In complex presentations, Review may continue iteratively as the plan evolves.
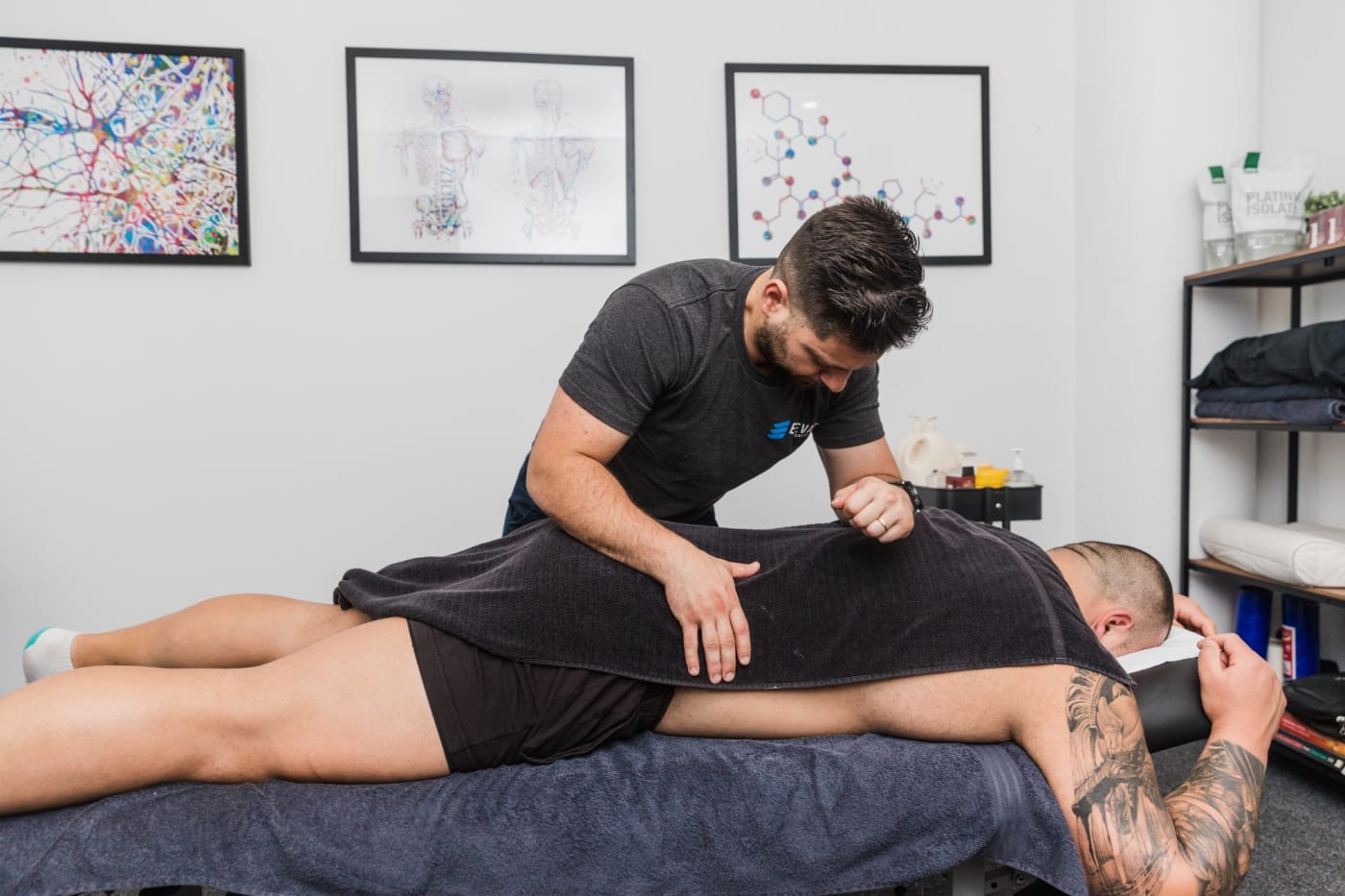
“Hands-on treatment to reduce pain, restore movement and begin recovery — with early active management from day one.”
Once we understand the problem, we address it directly. Restore is the hands-on phase — focused on reducing pain, calming the nervous system and returning normal movement. Pain education is integrated throughout, and early graded movement begins as soon as appropriate.
Goals
- Reduce pain to allow active rehab
- Restore joint range of motion
- Reduce muscle guarding
- Introduce early graded movement
- Build confidence in safe movement
What This Involves
- Spinal manipulation & mobilisation
- Soft tissue therapy & dry needling
- Pain neuroscience education
- Early range-of-motion exercise
- Activity & posture modification
Next stage when: Pain has reduced sufficiently to allow active, progressive loading — and the patient has enough movement confidence to engage with structured rehabilitation. Zero pain is not the criteria; sufficient function is.

“Progressive, individualised rehabilitation to rebuild your strength, load tolerance and movement quality — so recovery holds.”
This is where lasting recovery happens. Rebuild is the active rehabilitation phase — building the physical capacity that protects you from re-injury. The focus shifts from passive treatment to criteria-based progressive loading, guided by exercise physiology alongside physiotherapy and chiropractic.
Goals
- Rebuild strength & load tolerance
- Restore functional movement patterns
- Develop neuromuscular control
- Build task & activity confidence
- Reduce dependence on passive care
What This Involves
- Progressive resistance training
- Motor control & stability work
- Sport or task-specific training
- Functional movement retraining
- Graded return to sport or work
Next stage when: Functional milestones have been met — typically a defined level of strength symmetry, movement quality and activity tolerance, assessed through objective testing.

“Rediscover your passion for movement. Get back to the activities you love — from everyday tasks to the pursuits that make life feel good.”
Reignite is about rediscovering what movement means to you. Whether that’s returning to sport, keeping up with your kids, getting back to the gym, or simply moving through daily life without limitation — this stage reconnects you with the activities that make life feel good. Energy, confidence and enjoyment of movement are the markers of success here.
Goals
- Return to sport, work or daily activities
- Rediscover enjoyment and confidence in movement
- Establish consistent exercise habits
- Reduce recurrence risk
- Build the foundation for Stage 5 Resilience
What This Involves
- Performance & conditioning programming
- Return-to-sport validation testing
- Long-term exercise programme design
- Load management education
- Optional periodic maintenance reviews
Graduation when: The patient has met their stated goals, established independent management strategies, and has the confidence and capacity to maintain their progress. Not all patients need this stage — it is an additional layer for those with performance goals or complex long-term needs.

“The final stage is where lasting change is made — building a body armoured for life, and a confidence that extends well beyond the clinic walls.”
Resilience isn’t just about being pain-free — it’s about building a body that can withstand the demands of life, recover faster when challenges arise, and continue to grow beyond what brought you through our doors. We work with you to establish sustainable habits, independent movement practices and a mindset of ongoing development. This is where the clinic becomes a place to challenge yourself, not just recover in.
Goals
- Build a body armoured for long-term life demands
- Establish independent movement and training habits
- Develop lasting confidence in your own body
- Create a framework for ongoing growth and development
- Build longevity beyond the clinical relationship
What This Involves
- Sustainable self-management strategies
- Independent exercise programming
- Periodic check-ins and progress reviews
- Education on body awareness and injury prevention
- Goal-setting for continued growth and challenge
This stage marks the completion of the Dynamic Resilience System™ — but for many patients, it’s just the beginning of a new relationship with their body and their health.
Your journey through the system
The DRS is a framework, not a protocol. No two patients move through it in exactly the same way — and that is by design.
Not always linear
A patient progressing well in Rebuild may experience a flare-up that temporarily shifts focus back to Restore. This is the system working as intended — adapting to you, not the other way around.
Not every stage for every patient
Straightforward presentations may reach their goals at the conclusion of Restore. Athletes seeking performance optimisation may enter directly at Rebuild or Reignite. The entry and exit point is always based on your specific needs.
Criteria-based, not time-based
You progress when you have met measurable clinical milestones — not when a fixed number of sessions has elapsed. Treatment is always calibrated to where you actually are, not where a schedule says you should be.
One coordinated plan
Physiotherapy, chiropractic and exercise physiology work together within a shared framework. No conflicting advice, no gaps between disciplines, no starting from scratch each time you see a different team member.
The whole person, not just the symptom
Sleep quality, psychological stress, fear of movement and lifestyle demands are assessed from the outset and factored into your plan. These are not secondary considerations — they are primary drivers of recovery.
Toward independence
The goal of the DRS is not to create dependency on treatment. It is to give you the knowledge, strength and confidence to manage your own physical health — with clinical support available when you need it.
Explore our services
The Dynamic Resilience System™ is delivered by our integrated team of chiropractors, exercise physiologists and massage therapists across Bella Vista and Earlwood.